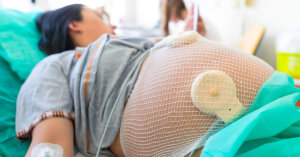
What is induction or induced labor?
The onset of labor is a normal physiological function at the end of pregnancy. Unfortunately, sometimes there is a legitimate health concern which requires labor to get started before nature begins the process on its own. This forced early labor is known as induction.
Induction can be brought about by several different methods, such as medical drugs, breaking the membrane surrounding the amniotic fluid, or by home remedies and alternative modalities.
Why do doctors and midwives induce labor?
- The mother has a health condition which poses significant risks to herself and/or the baby if the pregnancy continues (InterUterine Growth Retardation (IUGR) for instance)
- The pregnancy has lasted more than 42 weeks (though some doctors move this time limit up to 40, or even 39 weeks)
- The baby isn’t moving well in the kick test (10 kicks in a two-hour period when the baby is usually active)
- The ultrasound-based biophysical profile finds possible signs that the baby isn’t growing well
- Though studies don’t support it, there is a widely held belief that induction might prevent shoulder dystocia by not allowing the baby to grow larger than 8 lbs., 13 oz.
- A hospital routinely induces labor based on trends and profits
What most first-time pregnant women don’t know is that, on average, labor starts naturally at 41 weeks and 1 day. This is well after many doctors wish to induce these days.
“The timing of planned birth is potentially modifiable, and the benefits of waiting should be communicated to clinicians, mothers, and families,” says study co-author, Dr. Jonathan Morris of the Kolling Institute and the University of Sydney.
Reasons why you should induce
There are many good reasons why an induction may be necessary:
- Inducing labor can be beneficial when a pregnant woman is sick. For instance, if a woman has uncontrollable high blood pressure or the baby is clearly showing signs that the placenta is not functioning well, this is often the best option.
- Induction can also be viewed as a way to avoid infection if the amniotic fluid membrane (sac, or “waters”) has broken.
- Some women are so uncomfortable in late pregnancy that they are actually suffering. Induction can become very attractive in this case.
- It is popular to induce labor rather than let the pregnancy go beyond 42 weeks. The concern is the placenta may not continue to function well.
Maintaining the support of one’s birth team
Women might feel more inclined to accept induction if the midwife or family practice doctor can’t or won’t help her after 42 weeks gestation. This “rule” to limit pregnancy to 42 weeks or less varies among practitioners, so be sure to discuss your options with your midwife or doctor.
Induction can be tempting for a variety of social and familial reasons as well, such as:
- To ensure that your doctor or midwife will be on hand (they may have an upcoming vacation planned)
- Wanting to have the baby while a husband, partner, or other special person is in town (perhaps on military leave)
- To avoid having a baby on the day of a final exam or during an important family event
- Before insurance coverage changes
How can I know when an induction is medically necessary?
A test called a “biophysical” exam can be done using an ultrasound machine to assess fetal well-being by looking at fetal movement (including swallowing), amniotic fluid levels, blood flow through the cord, and other characteristics. These tests seek to determine whether the pregnant woman or fetus are so sick that their chance of death outweighs the side effects and risks of induction.
If they are that sick, then induction becomes a tool for maintaining their well-being. This test can be repeated as needed, but it isn’t perfect. Some providers induce even with good test results.
Reasons why you should not induce
On the other hand, there are also plenty of reasons why induction may not be the best choice.
- Even a 35-36 week gestation baby (just 1-2 weeks earlier than what is considered full-term) has a 1% higher chance of dying in the first year of life than a full-term baby.
- Sometimes induction methods work really well, while other times it takes days to get the labor to start because the mother and baby just weren’t ready.
- Some inductions still end in cesarean. If the birth team is patient, the induction may still work without a cesarean even if it does take several days.
- Induction is often associated with several other interventions. The more interventions there are, the less mother-infant skin-to-skin time may occur, as the baby is more likely to need resuscitation.
- Epidural anesthesia can be avoided with induction, but it is a common expectation for a woman to have an epidural if they are being given Pitocin (Syntocin), as if the two are a set.
- Medications can come on strong for some women, and the side effects may be severe enough to make a cesarean happen. Finishing the labor with a sudden cesarean is more likely during labor that is induced with medications.
- Hormones are very important and induction by Pitocin doesn’t release maternal hormones to prepare the brain for loving a dependent baby. Induced women may need extra support during and after birth.
- Strong contractions from induced labor can pile up and block the baby’s recovery time between contractions. Natural labor is sometimes super strong and contractions can be close together too but aren’t as likely to reduce the baby’s oxygen levels as much.
Sometimes the fuss over whether or not to induce labor wears a woman out mentally. She expects a baby soon after the induction starts, but it’s not uncommon for induction to take up to three days.
Fortunately, the IV Pitocin, prostaglandin on a string, and herbal drops can be stopped at any time if a woman needs to rest, if they aren’t effective, or if they’re too overpowering. Cytotec can’t be stopped though, and that’s a big problem with that popular inducing agent.
The good news is, there is an ongoing movement to lower the number of unnecessary inductions in the United States. The March of Dimes is on a campaign to reduce inductions to only those most medically necessary and to not induce before 39 weeks.
If you’d like to learn more, here is a link to the Coalition for Improving Maternity Care’s Induction Fact Sheet listing the many risks of induction.
How inductions are done
Natural induction
There are a variety of natural means to induce. Induction of labor can be started by natural means when a substance supports something that the mother needs. For instance, acupressure supports circulation of the mother’s own hormones, which can trigger induction.
Special foods, walking, lovemaking, nipple stimulation, herbs, homeopathy, body work, moxibustion, and body work may all sometimes bring on labor.
Castor oil is a classic home remedy as well. There are many ways to use it—with orange juice or root beer, as oil to cook eggs in (using more than the normal amount of oil), or simply straight up. The texture is very oily and some women do gag, but combining it with a preventative homeopathic seems to help. Just make sure to eat breakfast first, about 45 or 60 minutes before using castor oil. Oatmeal or another cooked grain makes for a good base in your stomach.
There is a way of blending homeopathy and herbs that seems more effective than either alone. Acupuncture seems effective too, especially when done by a very experienced acupuncturist.
I prefer natural methods, and take self-induction very seriously. I think that a natural induction can be worth a try before a medical induction when the healthy mother is motivated to try it and she is open about it with her birth team.
Exceptions to why inducing naturally may not work
Most often, inductions fail because either:
- The baby isn’t ready yet (being 40 weeks pregnant doesn’t mean every baby has released the special proteins and other signals of readiness), or
- The baby is not engaged in the pelvis.
Note: Don’t ever induce yourself without first talking with your care provider and making a plan. Because natural ways can also have side effects, I can only recommend using them with the support of a skilled practitioner.
Medical induction
Medications are generally effective more often and earlier in pregnancy than natural means. Medical supervision and a hospital stay with monitoring for mother and baby will reduce the risk of contractions that are too strong and too close for good oxygenation between contractions, or rupture of the uterus.
Pitocin is given with IV fluids through a catheter in the arm or hand. “Prostaglandins” are the artificial hormones used here. The gel is put on the cervix to ripen it and sometimes labor can start from just a few applications.
Another form is by a very inexpensive pill called Cytotec. Though often effective, it is associated with high rates of ruptured uteruses, amniotic fluid in the mother’s lungs, shock, and/or maternal death.
What about releasing the membranes?
One medical way that is sometimes thought to be a “natural way” (and that makes me rather uncomfortable) is breaking the water, also known as rupturing the membranes. A plastic hook is inserted through the cervix to snag the membranes and make a leak or a gush.
If labor is slow, breaking the water slows labor more. If labor is (or would be) fast, breaking the water may speed labor up.
In my opinion, babies born in the sac seem the most alert and peaceful—they’ve had an internal water birth after all! The intact sac is useful to put a thin cushion of fluid between their head and their mother’s pelvis with the contraction making a thin stream of water between them and assisting rotation.
A calm doula is a good addition to any induction. She should know the psychology of comfort, encouragement, and patience to be with a woman from before the induction has begun all the way through to the birth. Two doulas will allow them to tag team for potentially longer inductions, such as first babies, inductions before 41 weeks, and inductions when the baby is not yet engaged in the pelvis.
The Spinning Babies® view on induction
The first question I ask at Spinning Babies® is: What position is your baby in? I don’t see the point in trying to induce a posterior baby. Help the baby get better flexion, get into the anterior or left transverse position, or at least applied to the cervix. Then within 24-48 hours labor generally starts.
Pelvic balancing to help the pelvis become more stable may add quite a bit of comfort as well. Engagement matters, and if you’re overdue, engagement matters even more if the mother has given birth before.
Helping the baby engage through pelvic and uterine alignment (balancing) often starts labor once a woman is overdue and when the baby hasn’t been engaged previously. If a first baby is OP or ROT, please do everything you can to balance the body and engage the baby first.
When doulas and midwives have asked my advice about natural induction methods, they are often surprised to hear me turn away from herbal tinctures and focus on the baby’s position and station. I want to know if the baby is engaged. Other than the baby is fully grown and ready for birth, that’s the most important thing for labor to start on its own.
What about cervical ripeness?
I don’t care how much the cervix is dilated. If the cervix hasn’t been cut to take a sample for the lab, then body balancing will help it ripen when the time is right. I care about how the baby is presenting. If you help the baby to position, the rest will happen by itself!
Might the baby be ready even if labor hasn’t started?
An exception to our saying, “Babies come when they are ready” maybe when there is hypertension in pregnancy. Metabolism can be “sloshy” due to the cause behind the fluid retention, a slight rise in blood pressure, and the subtle malnutrition that goes with it. The mother’s body may not pick up on the baby’s signals to start labor. This is my ‘lay’ explanation for what I see when labor onset is missed and babies are indeed overdue.
Emotional reasons for labor onset to be delayed are usually immense stressors and not just normal stress. But an “airing out” day is a good thing, too. Sometimes there’s just too much time to ponder the “reasons” why the baby may not be coming that women who give birth earlier in gestation don’t have. Every situation is different, but generally, providers should be more reluctant to find fault with the woman’s head – at least not before investigating the baby’s head (position)!
Laboring with an induction
Since Pitocin (syntocin) doesn’t cross into your brain to alter your perception of pain in labor, induced labors can actually be more painful. Fortunately, there are techniques you can do to take the edge off the pain in an induced labor:
- Pelvic floor (side-lying) release (repeat every four hours)
- Abdominal release
- Side-opening stretch and/or psoas release
- Keep the lights low and reduce mental stimulation as much as possible (TVs, debates, worry, family gatherings in your room, computer time, etc.).
- Increase rubbing, massage, loving touches, smooching, cooing, and other loving expectations of meeting your little one together with your loved one(s).
- Get a good doula who knows how to talk calmly to you, your loved ones, and the staff.
- Do slow and long massage strokes in a quiet, dark or dim room.
- View Spinning Babies® Parent Class to learn the common stalls of labor progress and what to do about them.
It’s often effective to start Pitocin at a half-dose and bring it up more slowly than a typical in-and-out schedule for a busy hospital. Negotiate with your doctor and remind the nurses. Ask to speak to the doctor/midwife if the labor contractions come on too fast and hard. The dose can be slowed by the nurse at the provider’s instruction.
Realize that contractions will get harder before the amount of dilation that is required is reached. At 4 cm, contractions maybe 90 seconds long and 2.5 minutes apart for a while, and then the cervix dilates to 5 cm. In spontaneous labor, contractions must get quite strong and close together to give the induction “permission” to get you past 8 cm.
You have to change the way you look at the induction. Instead of seeing it as something done to you, try looking at it as a tool you have chosen—or allowed to be used—to bring your baby to you. Seeing our life events as being within our control makes life more manageable and satisfying.
Final thoughts on induction
It’s possible that with an induction, your instincts don’t match the induction care plans. Talk to your providers and nurses about your desires as an equal. If you agree to induce, make the induction work for you by seeing it as a tool and using the comfort measures in this article. And remember, the risk of not inducing should always be equal or higher than the risk of inducing.
In the end, induction decisions are parenting decisions. You are the mama—you get to pick!