Head’s up! A breech baby has their buttocks coming into mother’s pelvis before the head. Usually, the buttocks will be born first, less often the feet or knees emerge first.
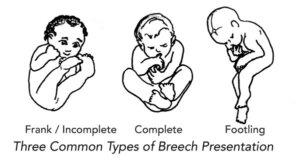
What are the types of breech positions?
Is breech presentation a malposition or a normal variation?
When is vaginal birth safer than surgery and when is a cesarean better?
Suggest your doctor, midwife, or or other person on your birth team to expand their spatial skills to identify and gently help a stuck breech baby’s safe vaginal birth by taking Gail Tully’s unique online Breech Basics Course.
Unfortunately, some skilled sonographers, midwives, and physicians may write “breech” in the chart when the baby is in an oblique (diagonal) or transverse lie because the baby isn’t head down. Our suggested activities to help an oblique or transverse (sideways) baby become head down can be very successful.
The specific causes and solutions for oblique or transverse lie positions may differ in some ways and may be the same in one way compared to a breech baby.
If you baby is indeed breech, we offer three ways for parents and providers to learn how to help their baby turn head down:
1. We have plenty of articles, tips, and tricks on our website, and the best part is they’re FREE! Here are some to get you started:
2. Helping Your Breech Baby Turn
Start during your 32nd week of pregnancy (or right away if 34 weeks or later) with our convenient ebook. Follow along with our structured program or adapt it to fit your needs. Give your baby room to turn head down on their own, or reduce muscle tension before an external cephalic version (ECV, the doctor turns the baby).
3. Our Spinning Babies® Parent Class
This streaming video walks you through our basic recommendations for helping all babies be in a more ideal head-down position. There’s even an additional scene showing Gail help a pregnant couple use the Breech Tilt position on an ironing board from that class included in our Flip-a-Breech page.
In my experience, most babies are breech due to uterine ligaments and muscles being either too tight and asymmetrical (twisted or torqued) or too loose. This would be in the “imbalance” category. Imbalance can happen to anyone but can also be balanced with repetitions of balancing activities. Examples of imbalance are common enough but can contribute to a breech (or posterior) position:
Some midwives will say that breech babies may be breech because they want to be. That may be, but I suggest we address a possible imbalance of the uterus. I believe the baby will get in the best position possible given the space in the womb.
It’s not that any woman isn’t perfect inside, but optimal room in the uterus depends on pelvic alignment and ligaments of equal length. An imbalance may be restored if a woman has the right technique and help for her body.

Baby’s breech position can be a normal response to the shape of the space inside the womb. Usually, the womb is aligned to encourage the baby to be head down. Whether or not it’s normal that any particular breech baby isn’t head down varies, just like the ease around head down babies varies. Not all head-down babies have easy births, and not all breeches have difficulty.
As long as the baby is able to complete the rotation and movements for breech birth (commonly called the Breech Cardinal Movements), and there are no malformations of the baby or the mother that might interfere, breech birth may be natural and normal. Most of the time, a breech baby can be born vaginally and quite safely.
Most breech babies, just like head-down babies, tuck their chins and come out in a tube shape. When the baby’s head is tucked in like this, making the baby rather tube-shaped, then breech is actually a fine position for birthing a full-term baby naturally.
An ultrasound in early labor or close to the baby’s due date can verify head position at that time. It is now thought by experts that if the baby’s head has been looking up during pregnancy, a cesarean is the best choice. If the head is looking straight (neutral) or down (flexed), then the chin can tuck itself or be tucked by the breech-skilled provider and a vaginal birth can be a safe option.
The baby’s head and arm position can certainly change in labor. A mother, parent, doctor, or midwife can’t always predict which baby will come easily or get stuck. If the baby gets stuck, it is too late to do a cesarean. But it’s not too late for a breech-smart expert to correct the problem by immediately rotating the arms free and flexing the chin so the head can fit the pelvis. These skills are rare but once learned will save lives.
Few doctors have proper training in breech skills, and many midwives are untrained as well. There is misunderstandings in being hands-off or hands-on but much confidence among providers who may have taken a workshop but not have much experience. You might look towards either of the far ends of the spectrum to find providers with breech skills. For instance, the chief of staff of Labor and Delivery at a big hospital or a country doctor, or even the rare, breech-skilled home birth midwife.
A childbirth educator, birth activist, or doula might have the name of someone with breech skills as well. Ask in an online forum like
Some women and couples travel long distances to a doctor or midwife experienced in natural breech birth. Names are not likely to be put on the internet with the current fear about breech vaginal birth and the risk of potential legal actions. Even when breech birth goes well, midwives and doctors can face serious opposition from their peers for supporting vaginal breech birth.
What makes a person experienced with breech birth?
Is it helping at a certain number of breech births? Is it knowledge of the physics and cardinal movements of breech birth? Is it knowing when to keep your hands-off and when/how to hands-on without pulling? The answer is: all of the above.
Here are a few standout candidates from several countries of the world that check off all of the breech birth boxes:
As you search for a provider to help you, whether they have a degree/reputation or not, ask them to show you how they release stuck arms or a trapped head. If they can’t readily do this with a doll and pelvis (or another prop), then keep looking. They may be nice, sincere, and skilled—just not in breech.
I have seen home and hospital providers not know how to free a trapped baby, even with many successful breech births behind them, because it had always been easy up until then. Breech birth can go well, but when it doesn’t, more babies die because the over-confident provider really didn’t know what to do. I don’t mean to be negative here, but saying this straight can help parents choose a provider who knows well how to save a life.
We are living in a time when expert breech providers are gathering and sharing ideas and data. Three different studies show the benefits of an all-fours/knee and elbow position for pushing in the last phase of a breech vaginal birth.
The biggest problem with breech position is the lack of experience in the person catching the baby.
Pulling on the baby or waiting without seeing clear fetal rotation or descent can cause severe injury or death. A vertical birthing position fits nature’s design for safe birthing. When a mother is standing, sitting up on a higher style birth stool, or in a hands-and-knees (or knee-elbow) position, the baby can more easily rotate through the open pelvis. There will still be need for skills because birth position does not prevent the chance baby gets stuck, but it does reduce the chance.
Breech birth on the birthing person’s back is not very safe, as the baby can’t help with the birth very well. Gravity pulls the baby into the mother’s back and not out her vagina. The mother’s sacrum is pressed by her weight into the bed and a doctor or midwife is more likely to pull, even gently—which is bad. Breech itself may not be a malposition, but requiring a woman to lay on her back is definitely a malposition for birthing!
Stuart J. Fischbein, MD, wrote, “…there is enough wisdom and evidence to suggest that when properly chosen, women can have better outcomes with vaginal deliveries and babies are no worse off. Actually, knowing what we do about the microbiome, epigenetics, and bonding, a vaginal birth is really much better, but those things are never considered in the medical model.”
Rixa Freeze, PhD, and David Hayes, MD, have dedicated their lives to educating as many birth professionals about physiological breech birth and the history of breech tools and techniques and the published and well known physicians and midwives promoting breech techniques they developed. See Breech Beyond Borders for their classes.
Spinning Babies® online and in person classes are:
We also have a page on if your breech baby doesn’t turn, because sometimes a breech baby remains breech in spite of our best efforts to make room for baby to turn.
Most breech babies today are born by cesarean surgery. Though obstetricians in the U.S. now consider breech to be too dangerous for vaginal birth, at some university hospitals in Norway, France, and Canada, the safety of vaginal breech birth is well proven. Dr. Louwen’s extreme knowledge of breech birth cardinal movements and knee-elbow position techniques have been proven to be safer than cesarean breech birth in his Frankfort hospital.
The techniques to help the arms and head of a breech baby are similar, whether in a vaginal or surgical birth. If delivering a breech baby, a doctor has to figure out how to get the chin tucked and past the mother’s bones, or through the tight abdominal incision.
The same techniques that may help a breech baby flip (body balancing and Forward-leaning Inversion) will help a woman’s soft tissues be ready for any vaginal birth, as well. The womb will be more in line with her pelvis and her pelvis with her pelvic floor, and there will be less tension and more function in the muscles.
However wonderfully we’re designed for birth (even breech birth), having a skilled attendant is necessary for the unexpected. You can read more in Mary Cronk’s article, Keep Your Hands off the Breech. Mary did use a more “hands-on” approach though when the baby hadn’t rotated or flexed the head, and requires gentle, expert help.
Surgery has reached an accepted level of safety because of improvements to surgical techniques, blood replacement procedures, and antibiotics to treat all too common, post-surgical infections. Major surgery has risks for the mother, however, such as blood loss, anesthesia, and infection.
For the baby, being born cesarean doesn’t mean being lifted up from the womb in the same way that they’re lifted up from a crib. Difficulty with the delivery of the arms and/or head can happen in a surgical birth too. The baby can still suffer an injury or death. The number of future siblings dying might even be equal to the number of breech babies saved by doing cesareans for almost all breech babies (Thomas Van Akker, MD).
Important physiological changes in brain development are now thought to occur during natural labor contractions. A scheduled surgery bypasses this physiology. Surgery can be life-saving when vaginal breech birth isn’t appropriate, but in a routine form the gut and brain are compromised without benefit to the child and the risks of surgery sometimes are significant to the birthing woman.
Here is a video of a lovely cesarean breech birth. I cried upon seeing the mother’s face when she saw her baby. It’s incredible how kind everyone is to the mother and child. Love is the most important thing that your baby is yearning for!
Consider whether it is reasonable to your health and whether your labor would allow you to reach surgery in time. This will give the baby a catecholamine surge to prepare for air-breathing (See The “Stress” of Being Born in Scientific American). Spontaneous labor might help protect against “late prematurity,” a growing risk due to increasingly scheduled births that turn out to be not as close to nature’s due date as was originally thought.
Some women will appreciate early labor for these advantages, while others will know that it is not feasible for them.
Discuss the possibility of labor with your doctor, and please don’t spring it on them without any warning. Sometimes delaying surgery until spontaneous labor is not wise, such as when the mom has a long distance to drive coupled with a previously fast birth or other health factors discouraging labor.
Healthy labor is good for healthy babies.
The early 2000’s brought with it an amazing examination of how breech babies are born. Early in the decade, the term “Breech Trial” (a nickname for the Mary Hannah study) recommended cesarean surgery for most breech births. But in examining the study, and adding more appropriate data with better interpretation, Hannah’s group found that qualified breech physicians were successfully swinging the vote in favor of vaginal breech birth.
Number 745 (Replaces Committee Opinion Number 340, July 2006)
Committee on Obstetric Practice has noted (and many other things
Note: This view does not reflect the view of experienced breech practitioners, such as Dr. Dennis Hartung of Wisconsin, for instance, who continues to attend natural breech births.
Dr. Robert Gagnon, a principal author of the new guidelines and Chair of the Society’s Maternal Fetal Medicine Committee, reported:
Breech pregnancies are almost always delivered using a caesarean section, to the point where the practice has become somewhat automatic. What we’ve found is that, in some cases, vaginal breech birth is a safe option, and obstetricians should be able to offer women the choice to attempt a traditional delivery…the society is also cautioning that many breech deliveries will still require a cesarean section, and that a vaginal birth is not recommended for some types of breech positions. In situations where a vaginal delivery is an option, the delivery should take place in a hospital setting. An experienced obstetrician should be present to attend the delivery and to offer a cesarean section if the labour does not progress smoothly or if complications arise.”
Dr. André Lalonde, Executive Vice-President of the Society of Obstetricians and Gynaecologists of Canada, said:
The evidence is clear that attempting a vaginal delivery is a legitimate option in some breech pregnancies.
Canada is following evidence-based logic in promoting the safety of many breech births. Still, the emotional setting of a birth also adds to safety. Calm, trusting patience and a vertical (hands-and-knees) position are still critical aspects of safety in breech birthing.
Note: This view doesn’t reflect that Canada is in great need of breech training for physicians and midwives to meet the needs of parents having breech babies. Women may not yet be able to find a qualified practitioner. Contacting the SOGC or Midwife Betty-Anne Daviss at UnderstandingBirthBetter.com may be helpful.
It’s good to compare the opinions of US and Canadian physicians on how a breech baby should be born. I was very interested in the experts’ teachings on physiological breech birth skills, so I put them into a brief picture book for providers who have been exposed to their teachings. You can find this Breech Quick Guide in our online shop.
For additional education to even further enhance your pregnancy and labor preparation, shop our extensive collection of digital downloads, videos, DVDs, workbooks, and more.
One of our most beloved products, now with subtitles in English, French, and Spanish, offering expert support to reduce intervention and increase comfort throughout pregnancy and birth.