Belly Mapping® and the Belly Mapping Method™ are born of the Spinning Babies® family.
Fetal positioning has a crucial impact on pregnancy comfort and ease in labor and birth.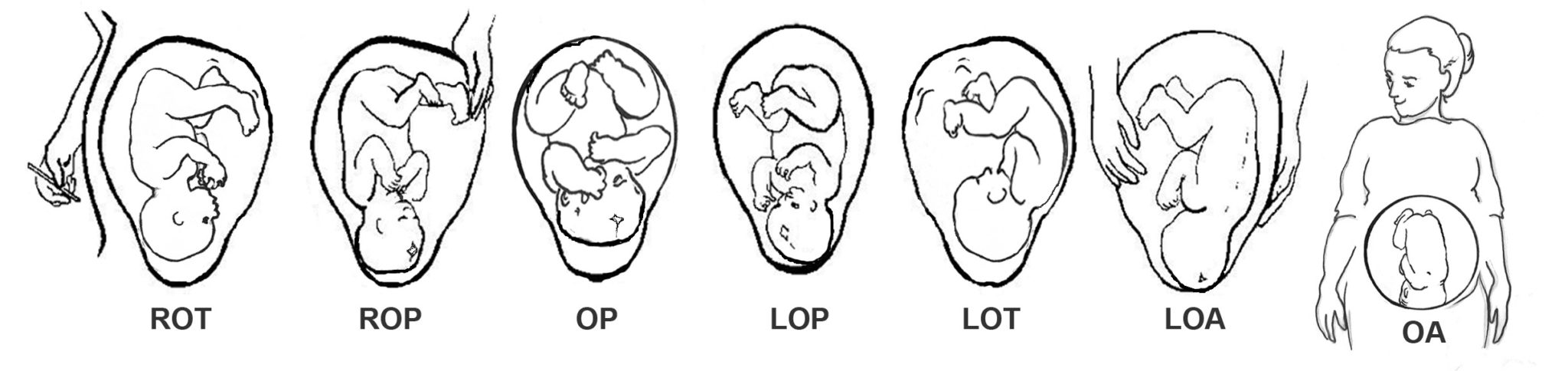
“Belly Mapping®: Using kicks and wiggles to predict posterior labor” appeared in Vol. 12 Issue 4 (Fall 2004) International Doula, a quarterly publication of DONA International (previously Doulas of North America). This was the first published material on Belly Mapping®.
Download the free Belly Mapping® parent handout.
The Belly Mapping® Method is a three-step process for identifying baby’s position in the final months of pregnancy. Parents can use the Belly Mapping® Method for their own enjoyment and education, while medical caregivers can use it to enhance their skills via visual clues. Doulas are able to suggest strategies for fetal repositioning when a posterior lie is suspected. The main goal of the Belly Mapping® Method is to enhance the parent’s ability to identify baby parts and to gain a sense of baby’s position.
Most people in the ninth month of pregnancy can tell without ultrasound if their head-down baby is facing right, left, front, or back. Some, however, find it hard to feel the baby through their belly. Firm tone, abundant amniotic fluid, a placenta on the anterior wall, or a well-padded tummy can all mute kicks and bumps from which to map baby parts.
If a mother hasn’t already, encourage her to take a day or two to learn her baby’s habits. She will notice more details about her baby’s movements when she is semi-sitting and breathing deeply and slowly.
 The Belly Mapping®️ Method can be a pleasant bonding experience for the family. You may increase your pleasure by allowing your exploration of your baby’s contours be imbued with love and acceptance. Judging whether a position is good or bad is a thought process, not an invitation to bonding. So, bring a breath of compassion and show up with open heart and open hands.
The Belly Mapping®️ Method can be a pleasant bonding experience for the family. You may increase your pleasure by allowing your exploration of your baby’s contours be imbued with love and acceptance. Judging whether a position is good or bad is a thought process, not an invitation to bonding. So, bring a breath of compassion and show up with open heart and open hands.
Fears about posterior fetal positioning are increased by thinking nothing can be done. Simple techniques taught in our Spinning Babies® Birth Preparation Online Course or viewed on our streaming video, Parent Class help reassure all of us that support is available to help baby turn through the pelvis in the birth process, if not before.
The “Three Anterior” babies have the easiest time rotating to the final birth position of Occiput Anterior. Babies in the anterior position can benefit from most of the same techniques we recommend by having less resistance or twists in the muscles lining the pelvis when the Three Balances and other techniques and birth positions are used.
Some posterior babies will descend well in labor. Most will take some time to rotate from posterior to anterior and then moving through the pelvis comes quicker.
Our free website resources include The Three BalancesSM and Dip the Hip, Standing Sacral and other techniques can make a huge difference. Birth positions choices to match where baby is in the pelvis can be crucial.

References
Simkin, Penny and Way, Kelli (1998) Position Paper: The Doula’s Contribution to Modern Maternity Care Position Paper Doulas of North America (DONA)
Simkin, Penny (1991)Just A Day in a Woman’s Life? Women’s Long Term Perceptions of Their First Birth Experiences, Part 1 Birth: Issues in Perinatal Care 18:4 December
Gardberg, M. and Tuppurainen, M. (1994) Persistent occiput posterior presentation – a clinical problem. Acta Obstetrics Scandinavia 73: 45-47
Fitzpatrick, M. et al. (2001) Influence of persistent occiput posterior position on delivery outcome. Obstetrics and Gynecology Vol. 98, No. 6, December
Ponkey, Susan et al. (2003) Persistant Fetal Occiput Posterior Position: Obstetric Outcomes. Obstetrics and Gynecology Vol 101, No. 5 part 1, May
Sutton, Jean and Scott, Pauline (1996 )Understanding and Teaching Optimal Foetal Positioning, New Zealand, Birth Concepts
Simkin, Penny and Ancheta, Ruth (2000) The Labor Progress Handbook Blackwell Sciences (See the expanded new edition published in 2005).
For additional education to even further enhance your pregnancy and labor preparation, shop our extensive collection of digital downloads, videos, DVDs, workbooks, and more.